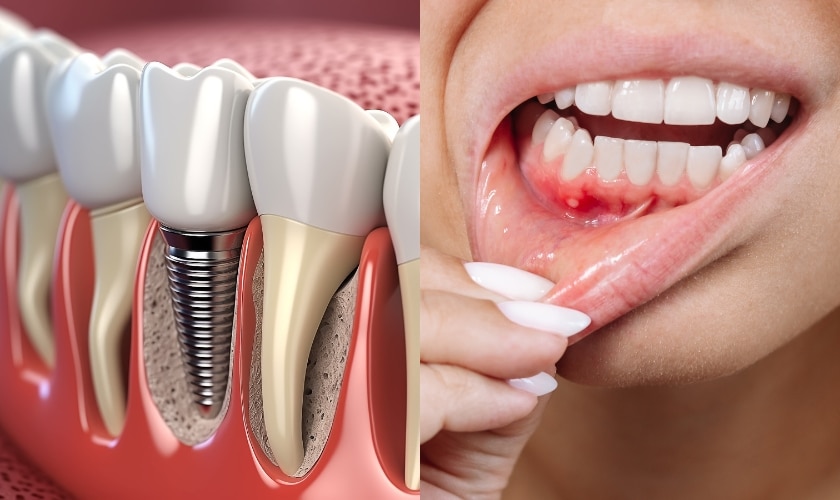
Dental implants are a remarkable innovation, offering a permanent and natural-looking solution for missing teeth. But before you embark on your implant journey, it’s crucial to understand the relationship between dental implants and gum disease.
What is gum disease?
Gum disease, also known as periodontitis, is a serious infection caused by plaque buildup around the gumline. It’s the leading culprit behind adult tooth loss, but the danger extends beyond your mouth. Gum disease has been linked to an increased risk of heart attack, stroke, and diabetes.
The scary part? Gum disease can progress silently, with no noticeable symptoms like bleeding gums or a receding gum line. That’s why regular dental checkups are vital. Early detection allows for prompt treatment, preventing complications like loose teeth and tooth loss.
Remember, healthy gums don’t bleed! If you experience bleeding gums while brushing or flossing, schedule a dental appointment to address the issue before it progresses.
What are implants?
Missing teeth can significantly impact your health and daily life. Dental implants offer a top-tier solution for replacing missing or damaged teeth. This innovative procedure involves placing an implant screw in your jawbone, essentially acting as a new tooth root. The implant is then topped with a natural-looking crown, bridge, or other restoration, creating a seamless replacement.
The best part? The final result looks and functions so naturally that no one will ever suspect you had a missing tooth! Here’s why dental implants are highly recommended: they prevent bone loss in your jaw, provide superior stability and durability compared to other options, allow for easier chewing and speaking, and achieve a flawlessly natural look.
Will you lose your teeth if you have gum disease?
We mentioned gum disease (periodontitis) as a major cause of tooth loss in adults. However, a diagnosis doesn’t automatically mean losing teeth. Early intervention is key! There are effective treatments and healthy habits you can adopt to reverse the infection and prevent tooth loss.
Severe gum disease damages the soft tissues supporting your teeth. This creates an opening for bacteria to invade deeper and ultimately destroy the jawbone that anchors your teeth. This is why tooth loss is considered the worst-case scenario for gum disease.
The good news? You can avoid reaching this stage. If you notice any signs of gum disease, like loose teeth, contact your dentist immediately for a checkup. Early detection and treatment can save your smile!
Does gum disease go away after a tooth is removed?
Losing a tooth to gum disease is a double whammy. While tooth extraction might seem like a solution, it doesn’t eliminate the underlying gum disease. In fact, untreated gum disease will continue to spread, potentially leading to further tooth loss.
Even tooth loss from unrelated reasons can increase your risk of gum disease. Missing teeth create spaces where bacteria can accumulate and weaken the surrounding gums and bone. This creates a vicious cycle, making the area even more susceptible to gum infection.
If you’re missing a tooth, replacing it is important. However, if you also have gum disease, it’s crucial to address the gum infection first. Treating these issues one at a time will ensure a healthy foundation for any future tooth replacement options.
Can you get an implant if you have gum disease?
While healthy gums are ideal for dental implants, gum disease doesn’t necessarily disqualify you. Remember how we explained gum disease weakens the jawbone and tissues? Even after treatment, these areas might not be strong enough to support an implant right away.
Dental implants require sufficient jawbone width and thickness for secure placement. Additionally, your gum tissue needs to surround the implant and its final restoration.
The good news? Procedures like bone and soft tissue grafts are common and successful. These grafts can strengthen your jawbone and gums, making you a much better candidate for dental implants. In fact, thanks to advancements in dentistry, very few people are permanently excluded from getting implants.
What happens if I get gum disease after an implant?
Getting dental implants doesn’t mean you’re immune to gum disease. Just like your natural teeth, implants require careful care to prevent peri-implantitis, another form of gum disease. This condition arises when plaque builds up around the implant, affecting the surrounding gum tissue and bone.
Here’s what to watch out for:
- Bleeding gums
- Swollen gums
- Bad breath
- A loose implant
In severe cases, peri-implantitis can lead to implant failure. The good news is that prevention is key! Here’s how to keep your implants healthy:
- Maintain a thorough brushing and flossing routine.
- Schedule regular dental checkups at least twice a year.
- Discuss preventive treatments with your dentist to stop bacteria before they become a serious health issue.
- Eat a healthy diet to support overall oral health.
- Avoid smoking or vaping, as they significantly increase the risk of peri-implantitis.
If you do develop peri-implantitis, there are treatment options available to control the disease and potentially save your implant.
A healthy smile starts with healthy gums. By addressing gum disease before pursuing dental implants, you’re setting yourself up for a successful outcome and a lifetime of confident smiles.